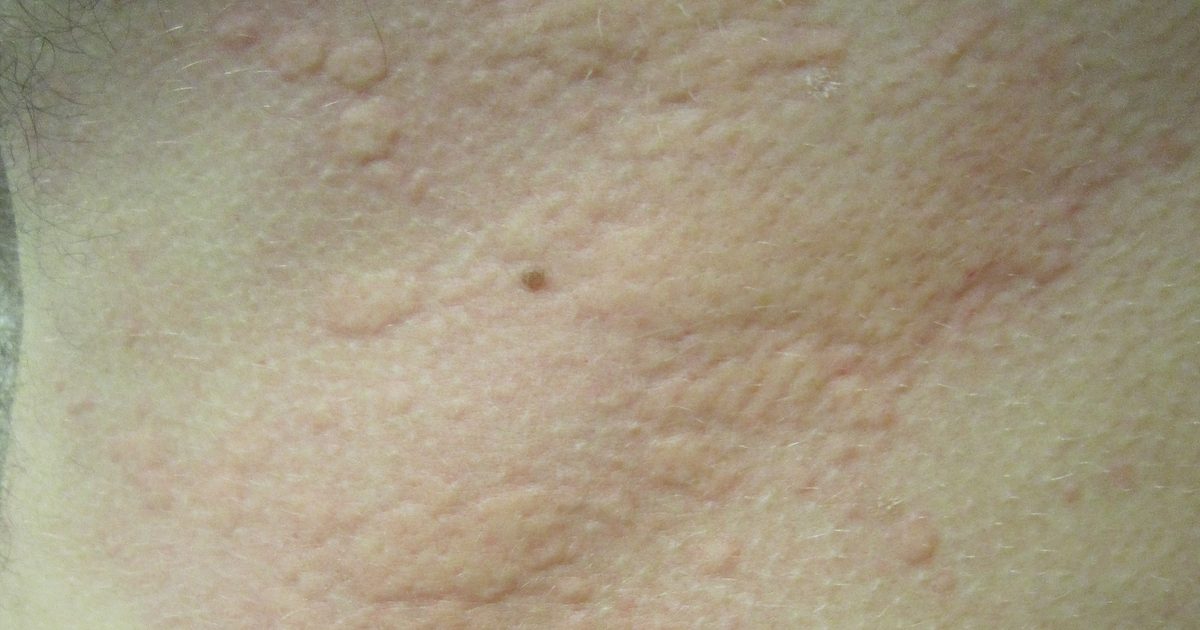
Imagine waking up with red, raised welts all over your body that itch intensely, appearing almost overnight without any apparent reason. You haven't eaten anything unusual, you haven't been in contact with anything new, yet your skin has erupted in angry hives. For many Indians, urticaria—commonly known as hives—is a puzzling and frustrating condition that can appear suddenly and disappear just as quickly, leaving people confused about what triggered it.
This comprehensive guide explains what urticaria is, why it's so common in India, how to identify it, diagnostic approaches, and most importantly, how to manage both acute and chronic cases.
What Is Urticaria (Hives)?
Urticaria, commonly called hives or wheals, is a skin condition characterised by the sudden appearance of red, raised, itchy bumps on the skin. These bumps can vary in size from a few millimetres to several centimetres and typically itch intensely—often far more than they hurt.
The hallmark feature of urticaria is that it appears suddenly and can resolve just as quickly. Individual hives usually fade within a few hours to a day, but new ones may continue to appear as the condition progresses, giving the impression that the rash is spreading.
Angioedema often accompanies urticaria. This is a deeper swelling involving the subcutaneous tissues, particularly around the eyes, lips, and throat. While urticaria affects superficial skin layers, angioedema affects deeper layers and can persist longer.
Two Main Types: Acute vs. Chronic
Understanding whether you have acute or chronic urticaria is crucial because management differs significantly.
Acute Urticaria lasts less than six weeks. It usually resolves spontaneously without treatment, though symptomatic relief is often needed. Most cases of acute urticaria in India are triggered by identifiable causes like food allergies, infections, or medications.
Chronic Urticaria persists for more than six weeks—sometimes for months or even years. In chronic urticaria, identifying a specific trigger becomes far more difficult. Recent Indian studies show that chronic urticaria affects 0.5 to 1.5% of the population and significantly impacts quality of life due to persistent itching and unpredictable flare-ups.
Why Urticaria Is Common in India
Several factors make urticaria particularly prevalent in the Indian population:
Tropical Infections: India's warm, humid climate is conducive to various infections—bacterial, viral, and parasitic—that commonly trigger urticaria. Infections like dengue, chikungunya, respiratory infections, urinary tract infections, and gastrointestinal infections frequently precede urticaria episodes. In fact, infections account for 30-50% of acute urticaria cases in India.
Allergenic Foods: Indian cuisine, while nutritious and flavourful, contains several common allergens. Seafood (particularly prawns), eggs, peanuts, tree nuts, and cow's milk protein are frequent triggers. Many Indians consume these foods regularly, making food-triggered urticaria more common than in populations with different dietary patterns.
Environmental Allergens: Pollen, dust mites, and mold spores are more abundant year-round in India's tropical climate. Air pollution—Delhi and many Indian cities rank among the world's most polluted—contains particulates that can trigger urticaria in susceptible individuals.
Medications: Common medicines prescribed in India can trigger urticaria. Antibiotics (particularly penicillins and sulfonamides), NSAIDs, and aspirin are frequent culprits. Many Indians self-medicate or obtain antibiotics without prescription, increasing exposure risk.
Autoimmunity: Recent research shows that approximately 30-40% of chronic urticaria cases are autoimmune in nature. In autoimmune urticaria, the body produces antibodies against mast cell receptors, causing the cells to release histamine spontaneously. This is independent of external triggers, making management different from allergic urticaria.
Symptoms and Presentation
Urticaria typically presents with:
- Red, raised welts (wheals) of varying sizes, ranging from a few millimetres to several centimetres
- Intense itching, often worse in the evening or after heat exposure
- Rapid onset, often developing within minutes to hours
- Transient nature: Individual hives fade within a few hours, though new ones may appear
- Angioedema: Swelling of deeper skin layers, particularly around eyes, lips, tongue, and throat—can be dangerous if the throat is involved
- Patterns: Hives may appear in lines if you've scratched, or may cluster together, forming larger erythematous areas
In acute urticaria, symptoms typically resolve completely within 24 to 48 hours of removing the trigger. In chronic urticaria, symptoms may wax and wane over months or years.
Identifying Possible Triggers
For acute urticaria, identifying the trigger is often straightforward. Common triggers include:
Foods: Seafood (prawns, fish), eggs, peanuts, tree nuts, milk, sesame, and mustard are the most common food triggers in India. Food additives and preservatives in processed foods can also trigger urticaria. The reaction typically occurs within 30 minutes to 2 hours of consumption.
Infections: Viral infections (dengue, influenza, colds) or bacterial infections (urinary tract infections, strep throat) can precede urticaria by several days. The urticaria resolves as the infection clears.
Medications: Antibiotics (penicillins, sulfonamides), NSAIDs (aspirin, ibuprofen, naproxen), ACE inhibitors, and statins are common culprits. If urticaria develops shortly after starting a new medication, discuss with your doctor about stopping or replacing it.
Insect Bites: Mosquito bites—extremely common in India—can trigger urticaria in some individuals, though true IgE-mediated allergy to insect bites is less common.
Physical Triggers: For some people, urticaria is triggered by physical stimuli:
- Dermographism: Hives appear in lines where the skin is scratched or stroked
- Cold urticaria: Exposure to cold water or cold air triggers hives
- Heat urticaria: Exposure to heat or hot showers triggers hives
- Cholinergic urticaria: Exercise or stress-induced sweating triggers small hives
- Solar urticaria: Exposure to sunlight triggers hives (rare but documented in India)
Psychological Stress: Emotional stress and anxiety frequently trigger or worsen urticaria in Indians, particularly during exam season, work pressure, or family tension.
Contact Irritants: Direct skin contact with certain substances like latex, nettles, or certain cosmetics can trigger urticaria, though true allergic contact dermatitis is more common than contact urticaria.
For chronic urticaria, identifying specific triggers is often impossible because the condition has become independent of external stimuli—particularly in autoimmune cases.
Diagnostic Approach
Clinical Diagnosis: A careful history and physical examination are usually sufficient for diagnosis. Your doctor will ask about the onset, duration, appearance, associated symptoms (angioedema, fever), potential triggers, and impact on daily life.
Allergy Testing: If a specific food or environmental allergen is suspected, skin prick testing (SPT) or specific IgE blood tests can identify IgE-mediated allergies. SPT is faster and cheaper; blood tests are useful if you're on antihistamines (which interfere with SPT) or have severe skin disease.
Infection Screening: For acute urticaria, blood tests may reveal infections like dengue (dengue IgM, NS1 antigen), influenza, or other viral infections that triggered the episode.
Autologous Serum Skin Test (ASST): In chronic urticaria, this test can identify autoimmune urticaria by injecting your own serum intradermally and observing whether hives develop. If positive, it suggests autoimmune mechanisms.
Thyroid and Autoimmune Screening: Since chronic urticaria is often autoimmune, thyroid antibodies (TPO, thyroglobulin), antinuclear antibodies (ANA), and other markers may be tested.
Complete Blood Count (CBC): A basic CBC rules out infections, parasitic infestations (elevated eosinophils), or other systemic conditions.
Faecal Examination: In India, parasitic infections (roundworms, hookworms) can trigger urticaria. A stool examination may be warranted in endemic areas or if eosinophilia is present.
Treatment Strategies
Acute Urticaria
First-Line Treatment: Antihistamines
Second-generation (non-sedating) antihistamines are the gold standard:
- Cetirizine 10 mg once or twice daily
- Fexofenadine 180 mg once daily
- Desloratadine 5 mg once daily
- Loratadine 10 mg once daily
These are preferred because they don't cross the blood-brain barrier and don't cause drowsiness. They're available across India at pharmacies and cost between INR 5 to 50 per tablet depending on brand.
If standard doses don't provide relief after a few days, doses can be increased up to four times the standard dose (e.g., cetirizine up to 40 mg daily in divided doses) under medical supervision. This is safer than switching medications.
First-generation (sedating) antihistamines like diphenhydramine or chlorpheniramine can be used at night if itching prevents sleep, but they're not ideal for daytime because they cause drowsiness and impair concentration.
Identifying and Removing the Trigger
Simultaneously, identify and eliminate the trigger:
- If a food triggered it, avoid that food for at least 6 weeks to allow sensitisation to decrease
- If a medication triggered it, discuss alternatives with your doctor
- If an infection triggered it, manage the infection
- If a physical trigger was involved (cold, heat, exercise), avoid that trigger
Supportive Care
- Apply cool compresses to itchy areas
- Avoid hot showers and bathing (stick to lukewarm water)
- Wear soft, loose cotton clothing
- Avoid scratching; keep nails trimmed short
- Avoid known irritants like cosmetics, perfumes, or tight clothing
Chronic Urticaria
Chronic urticaria requires a different approach because removing a trigger is often impossible.
First-Line: Second-generation antihistamines at standard doses. In chronic urticaria, the goal is to keep the patient itch-free throughout the day and night.
Second-Line: If antihistamines alone don't control symptoms adequately:
Omalizumab (anti-IgE monoclonal antibody): Particularly effective in autoimmune urticaria. It's expensive (INR 1-2 lakhs per dose in India) but highly effective. It requires multiple injections over several months.
Cyclosporine: Oral immunosuppressant used in severe, refractory chronic urticaria. Requires regular monitoring of kidney and liver function.
Corticosteroids: Used sparingly for short periods during severe flares. Chronic use carries risks of side effects.
Lifestyle Modifications
- Identify and avoid known triggers even if they're not the primary cause
- Manage stress through yoga, meditation, or counselling (stress is a major trigger in Indian patients)
- Maintain a symptom diary to identify patterns
- Avoid NSAIDs and aspirin unless absolutely necessary
- Ensure adequate sleep
- Avoid very hot or very cold environments if you're sensitive
Important Clarifications
Avoiding Unnecessary Dietary Restrictions: A common misconception in India is that urticaria patients must permanently avoid certain foods like milk, eggs, prawns, and brinjal. This is inappropriate and can lead to nutritional deficiencies. Food avoidance is only necessary if that specific food has been confirmed as a trigger through allergy testing and symptom correlation.
Urticaria Is Not Due to "Heat" or "Toxins": While heat can trigger urticaria in heat-sensitive individuals, urticaria is not caused by general body heat or accumulated "toxins." This common belief sometimes leads to unnecessary and ineffective treatments.
Autoimmune Urticaria Doesn't Require Dietary Modification: In autoimmune urticaria (where antibodies attack mast cells), dietary changes don't help because the trigger is internal, not external.
When to Seek Emergency Care
Seek immediate medical attention if:
- Angioedema involves the throat, tongue, or inside of the mouth (risk of airway obstruction)
- You develop difficulty breathing or swallowing
- You experience chest tightness
- You develop signs of anaphylaxis (severe systemic reaction with cardiovascular symptoms)
Tracking Your Urticaria
If you experience recurrent urticaria, keep a detailed symptom diary noting:
- Date and time of onset
- Appearance and distribution of hives
- Associated symptoms (itching severity, angioedema, fever)
- Potential triggers (foods eaten, stress level, infections, medications)
- Treatments used and response
- Duration of episode
Digital tools like MedicalVault allow you to store photos of your hives during different episodes and track your treatment responses over time. This record is invaluable for your dermatologist in identifying patterns and planning long-term management. Additionally, sharing your medical history with family members ensures that family members are aware of your triggers and can help manage your condition.
Key Takeaways
- Urticaria (hives) is characterised by sudden onset of red, itchy welts that typically fade within hours.
- Acute urticaria lasts less than six weeks and usually has an identifiable trigger; chronic urticaria persists longer and often has no clear cause.
- Common triggers in India include infections, food allergies, medications, environmental allergens, and stress.
- Approximately 30-40% of chronic urticaria cases are autoimmune in nature.
- Second-generation antihistamines are first-line treatment for both acute and chronic urticaria.
- Identifying and avoiding triggers is crucial for managing acute urticaria; for chronic urticaria, long-term antihistamine use may be necessary.
- Physical urticaria (cold, heat, pressure-induced) requires trigger avoidance and sometimes specific treatments.
- Unnecessary dietary restrictions are harmful and should be avoided unless foods are confirmed triggers through testing.
- Stress management is particularly important for Indian patients, as stress frequently triggers or worsens urticaria.
- Digital health tools like MedicalVault help track flare-ups and identify patterns over time.
If you experience recurrent urticaria or if symptoms significantly impact your quality of life, consult a dermatologist for proper evaluation, allergy testing if appropriate, and personalised treatment planning. Remember that urticaria, while annoying and uncomfortable, is rarely dangerous if managed appropriately, and most cases resolve completely with proper care.